Osteoporosis
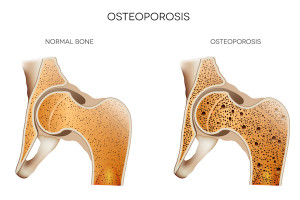 Osteoporosis is sometimes referred to as “thinning of the bones,” and it occurs when natural bone renewal or replacement doesn’t keep up with bone loss. Your bones become weak and brittle and even a mild injury can cause a bone fracture. This disease can affect anyone, but post-menopausal white and Asian women are at highest risk.
Osteoporosis is sometimes referred to as “thinning of the bones,” and it occurs when natural bone renewal or replacement doesn’t keep up with bone loss. Your bones become weak and brittle and even a mild injury can cause a bone fracture. This disease can affect anyone, but post-menopausal white and Asian women are at highest risk.
What are the Symptoms of Osteoporosis?
In general, the weakening of the bones does not cause any symptoms until the bone either breaks or cracks. This is especially true in the spinal column where the vertebrae can be crushed down just by the weight of your body. In this case you can experience:
- Back pain
- Loss of height
- Curved or stooped posture
In osteoporosis you are also at risk for bone fractures which require much less impact than normal. This is more common in the hip, spine and wrist.
What are the Causes and Risk Factors of Osteoporosis?
Normally your body continuously makes new bone and breaks down old bone. By the time you are about 20 years old, you have reached your maximum bone mass. Later, when the breakdown process exceeds the renewal process, then the bones begin to weaken. The risk factors for developing osteoporosis can be:
- Advancing age, female gender and a family history of osteoporosis all increase your risk for developing the disease. Also, if you have a small body frame (low bone mass) you are at increased risk.
- Hormones: Low estrogen level, such as after menopause, increases the risk for osteoporosis in women. In men treated for prostate cancer, testosterone levels can be low which also increases risk.
- Diet: A diet low in calcium increases risk as does a history of eating disorders such as anorexia.
- Gastrointestinal Surgery: If you had part of your stomach or digestive tract removed then you absorb less calcium from food. This can lead to osteoporosis.
- Medications: Chronic corticosteroid use (steroids, cortisone, etc…) can causeosteoporosis. Some medications used to treat depression, gastric reflux and cancer have also been associated with the development of osteoporosis.
- Lifestyle: Lack of exercise, excessive alcohol and smoking all increase your risk of osteoporosis.
Diagnosing Osteoporosis
For screening and diagnostic purposes, your doctor can take a bone density measurement. This test is easy and painless and usually measures the bone density in the hip, wrist and spine. If you have significant osteoporosis, the thinning of the bones can even be seen on a normal X-ray.
Treatment of Osteoporosis
The most common medications are the bisphosphonates. These can normalize the rate of bone turnover, increase bone density and decrease the risk of fractures. Your doctor might also recommend taking these medications along with calcium supplements and Vitamin D. Some versions of the medications even come with Vitamin D included. Examples of bisphosphonates are:
- Alendronate (Fosamax)
- Ibandronate(Boniva)
- Risedronate(Actonel, Atelvia)
- Zoledronic acid (Reclast, Zometa)
These medications can cause side effects such as:
- Nausea and abdominal pain
- Swallowing difficulty
- Inflamed esophagus or esophageal ulcers
The injectable forms of these drugs do not cause digestive problems.
Hormone therapy can help maintain bone density, but estrogen can also increase the risk of blood clots, breast cancer, endometrial cancer and maybe even heart disease. The drug raloxifene (Evista) generates the same effect as estrogen on the bone, and this drug carries less risk than hormone therapy.
In some cases you can’t tolerate the drugs listed above, or maybe they don’t work for you. In these circumstances your physician might try:
- Teriparatide (Forteo): This is a drug that stimulates bone growth much like parathyroid hormone. It is injected under the skin, and you take it for two years followed by treatment with a second drug.
- Denosumab (Prolia): Also used to build bone. It also comes in an injectable form given every six months. Denosumab can cause muscle and back pain.
Treatment also involves the prevention of falls. If you have poor balance, for example, you should begin to use a walking cane or a walker. Also, you might be advised to avoid using stairs.
Calcium, Vitamin D and Exercise
If you are between the ages of 18 and 50 you should get around 1,000 mg of calcium in your diet every day. For women over 50 and men over 70, the recommended amount goes up to 1,200 mg. Good sources of calcium are dairy products, dark green vegetables (like spinach), canned fish with bones (salmon and sardines), soy foods (soy milk, tofu) and calcium fortified foods. You can also take calcium supplements, but make sure your total calcium food and supplement intake does not exceed 2,000 mg.
Vitamin D allows for your body to absorb calcium, and vitamin D comes from skin sunlight exposure. However, if you are very seldom exposed to the sun due to being housebound or due to skin cancer concerns, then you should take a supplement. Ask your doctor about the best dosage for you.
Exercise is an important way to prevent osteoporosis. Weight bearing exercises are best, and just a brisk walk of up to 30 minutes a day can help prevent the disease.
Conclusion
Osteoporosis is a common disorder that leads to weakening of the bones and an increased risk of bone fracture. Diet, exercise and avoidance of tobacco and excess alcohol are keys to prevention. The diagnosis is made by bone density measurement, and many treatment options are available.


Recent Comments